Massage Matters
The Knot Whisperer Rides!

Monday, September 12, 2011
Does Your Weight-Loss Plan Include Massage? It Should!
Tuesday, August 16, 2011
Low-Back Pain Can Be a Pain in the Butt--Literally
Not only will 80–90 percent of the population have issues with low-back pain sometime during their adulthood but, in addition, back pain is one of the most common symptoms inducing people to visit a physician and is involved in almost a fourth of all occupational injuries and illnesses. In 2001, back injuries resulted in the highest percentage of short-term disability of all nonfatal illness and injury cases. In sum, back pain, especially low-back pain, is a big problem—for workers, employers, and insurance companies alike.
Part of the problem is that back pain can be difficult to diagnose, and physicians often overlook or misdiagnose trigger point pain (that is, localized areas of muscle soreness that refer pain to elsewhere in the body). This diagnostic difficulty can lead to treatments that don’t accurately address the problem, such as painkillers, which don’t necessarily rectify the problem but simply dull the pain. It is also worth mentioning that surgical rates for low-back pain are twice as high in the United States as in most other developed countries.
Often, to give a commonly occurring example, clients who are experiencing low-back pain actually have an issue with trigger points in the gluteal muscles, the piriformis muscle (which lies deep to the glutes), or even muscles as far away as the calf (the soleus muscle, to be exact). The piriformis, in particular, seems to be a major culprit when it comes to low-back pain. In my own practice, when I release knots in the piriformis muscle, I have had clients say they can feel the tension in their lower backs dissolve immediately. I even had one client say he felt his whole back realign when the tight spot in his piriformis let go.
Because low-back pain relief can be so close at hand—literally—it only makes sense to visit a knowledgeable massage therapist before trying something more invasive or simply palliative but not curative (such as pharmacologic “solutions”). And research is mounting to support this course of action. In one study, massage recipients reported less pain, depression, and anxiety, as well as improved sleep, and they showed improved trunk flexion. Stress hormones associated with chronic low-back pain were also reduced. A more recent study found similar results, with benefits lasting up to six months. And numerous other studies have shown massage to be helpful in relieving back pain.
Although reduction of stress hormones may come into play, in terms of how massage works to relieve low-back pain, as found in the one study, other researchers aren’t sure why massage seems to work. It may be that massage stimulates the muscle tissue locally or that it causes a response from the central nervous system. They also hypothesize that the reasons for improvement could be as simple as being in a relaxing environment or being cared for by a sympathetic therapist.
In any case, I agree with the chief author of the most recent study, who was quoted as saying, “If you’ve tried other things and you’re not getting adequate relief, then massage is a reasonable thing to try.” I would go one step further, though, and suggest that perhaps massage should be one of the first things you try.
Sources
Bagduk, Nikolai. 2004. “Management of Chronic Low Back Pain.” Medical Journal of Australia, vol. 180.
Bakalar, Nicholas. 2011. “Stubborn Back Pain? Try Massage.” New York Times, July 4 (http://well.blogs.nytimes.com/2011/07/04/embargo-july-4-5pm-for-back-pain-try-massage/?scp=1&sq=%22low%20back%20pain%22&st=cse).
Cherkin, Daniel C., et al. 2011. “A Comparison of the Effects of Two Types of Massage and Usual Care on Chronic Low Back Pain: A Randomized, Controlled Trial.” Annals of Internal Medicine 155:1–9.
Deyo, Richard A. 1983. “Conservative therapy for low back pain: Distinguishing Useful from Useless Therapy.” Journal of the American Medical Association 250:1057–62.
Deyo, Richard A., et al. 1996. “Low Back Pain: A Primary Care Challenge.” Spine 21:2826–32.
Hernandez-Reif, Maria, et al. 2001. “Lower Back Pain Is Reduced and Range of Motion Increased after Massage Therapy.” International Journal of Neuroscience 106:131–45.
Papadopoulos, E. C., and S. N. Kahn. 2004. “Piriformis Syndrome and Low Back Pain: A New Classification and Review of the Literature” Orthopedic Clinics of North America 2004 35:65–71.
Simons, D. G., and J. G. Travell. 1983. “Myofascial origins of low back pain. 3. Pelvic and lower extremity muscles. Postgraduate Medicine 73:99–105, 108.
U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention. 2004. Worker Health Chartbook 2004. Publication no. 2004-146. Cincinnati, OH: U.S. DHHS, PHS, CDCP, National Institute for Occupational Safety and Health. Fig. 1-38.
Sunday, August 7, 2011
Cruisin', on a Sunday Afternoon
A Jury of My Gears?
Saturday, August 6, 2011
Intersection of Terror!
August 6, 2011
Gabe Klein, Commissioner
Department of Transportation
City Hall
121 N. LaSalle Street
Chicago, IL 60602
Dear Commissioner Klein,
First, I want to thank you for all your advocacy on behalf of cyclists and pedestrians. As a regular bicycle commuter, I know the perils—and pleasures—of cycling on Chicago streets, and I very much appreciate all you’ve done to make such travel a little easier for Chicago’s citizens.
Now I’d like to direct your attention to an intersection that plagues me on a daily basis, that at Armitage, Elston, and Ashland. Going southbound on Elston on my bike, travel through that intersection goes without a hitch, but when I am going northbound, it gets a little dicey at the juncture between Ashland and Elston. Even when I am in the center lane, indicating, I would think, my intention to stay on Elston, cars routinely cut in front of me to turn right onto Ashland. Sometimes it is more treacherous than others, depending on how closely they cut me off.
What I’d like to propose is that the lanes on Elston south of Armitage be painted to indicate that those who intend to travel north on Ashland be in the right-hand lane and those traveling north on Elston be in the center lane; the far left lane is already marked for left turn onto Armitage. North of Armitage, I suggest that one of the two lanes that continue to Elston be turned into a bike lane. Ideally, I’d love a protected bike lane, but at this point I’d take anything that helped give bicyclists a clear right of way! Since this may be hard to understand in the abstract, I’ve created some drawings to illustrate what I mean.

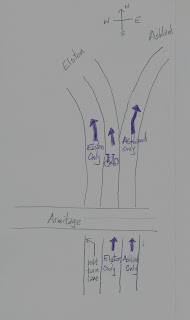
In the picture at right [above here, in the blog], I’ve used purple to show what I think should be painted onto the road.
If you have any questions about my concerns or suggestions, I hope you will feel free to contact me. I know everything can’t be attended to at once, but I hope this is a matter that you can investigate and resolve quickly.
Sincerely,
Brave Heart, Chicken Liver
Sunday, July 17, 2011
Massage Can Quiet Some of Dementia's Demons
“There are hardly any age-related conditions that cannot be improved with a weekly half-hour massage,” claims Sharon Puszko, owner of Day-Break Geriatric Massage Institute. Even a cursory look at current research on massage will verify the truth of that contention and, in fact, might suggest that there are few conditions, period, that wouldn’t be made better with massage. The value of massage as an intervention is especially high for conditions for which effective treatment continues to confound practitioners of conventional medicine, such as Alzheimer’s and other forms of dementia.
The loss of memory and, sometimes, speechlessness that characterize these conditions are a source of frustration for all concerned, both those afflicted with the condition and their caretakers. For those actually suffering from this condition, however, the frustration can result in agitation, of both a verbal and physical nature. Traditionally, such agitation has been managed either chemically (that is, with medication) or physically, with restraints, but neither of these methods has been shown to be especially effective.
The past decade, however, is distinguished by an increased interest in studying alternative treatments, including massage, for managing symptoms of dementia. These studies have made use of salivary (measuring levels of a stress-related amino acid protein), psychometric, blood pressure, and observational measures to assess the effects of massage on people with dementia. The treatments generally involved soft massage or therapeutic touch to hands or feet for short periods of time (10–20 minutes), accompanied by, in at least one study, the inclusion of aromatherapy.
Massage, in all cases, was found to have one or more of the following effects on the symptoms typically exhibited by people with cognitive impairment:
o reduced stress level
o less wandering/pacing behavior
o reduced physical agitation/aggression
o reduced verbal agitation/aggression
o lowered pulse rate
o less inappropriate behavior
o less resistance to being cared for
Study of the effects of massage on those troubled with dementia is still relatively new, however, so it’s hard to know exactly how powerful the calming effects are. But the results are definitely promising. In the meantime—until more research has been conducted—since none of the existing studies have found massage to have any negative impacts on those with Alzheimer’s or other forms of dementia, massage seems like a useful nonpharmalogical tool for helping to cope with some of this impairment’s most disruptive symptoms.
Also, if you are inclined to believe the old adage An Ounce of Prevention Is Worth a Pound of Cure, listen up! A recent study found that those suffering from depression may nearly double their risk of developing dementia later in life. Lead author of the report, Jane Saczynski, says, “While it’s unclear if depression causes dementia, there are a number of ways depression might impact the risk of dementia. Inflammation of brain tissue that occurs when a person is depressed might contribute to dementia. Certain proteins found in the brain that increase with depression may also increase the risk of developing dementia. In addition, several lifestyle factors related to long-term depression, such as diet and the amount of exercise and social time a person engages in, could also affect whether they develop dementia.” But as I discussed in my article “Turn That Frown Upside Down: In a Massage Face Cradle,” massage has been found to help regulate some of the biological causes of depression.
Massage may also be able to intervene in the onset of dementia is helping individuals maintain their overall health: a study published this week in Neurology provides evidence that when small health problems are added up, a person’s risk for dementia increases. In fact, for each small complaint a person has as they age—from sinus issues to hearing problems and bad dental health—the risk for dementia increases by 3 percent. For instance, those who had no health complaints at the start of the study had an 18 percent risk of developing dementia over the next ten years, whereas someone with eight minor health complaints had a 30 percent risk and those with a dozen complaints showed an increased risk of 40 percent.
Massage, of course, can’t insure that someone won’t develop dementia. But given that massage has been shown to improve a variety of mental and physical health conditions, it can certainly be another tool in your arsenal to help maintain your health. So after you have that apple today to keep the doctor away, get on the phone and schedule a massage!
Sources
Hansen, N.V., T. Jørgensen, and L. Ørtenblad. 2006. “Massage and Touch for Dementia,” Cochrane Database of Systematic Reviews, no. 4.
Hawranik, Pamela, Pat Johnston, and Judith Deatrich. 2008. “Therapeutic Touch and Agitation in Individuals with Alzheimer’s Disease,” Western Journal of Nursing Research, 30:417–34.
Holliday-Welsh, Diane M., Charles E. Gessert, Colleen M. Renier. 2009. “Massage in the Management of Agitation in Nursing Home Residents with Cognitive Impairment,” Geriatric Nursing, 30:108–17.
Moyle, Wendy, et al. 2011. “Exploring the Effect of Foot Massage on Agitated Behaviours in Older People with Dementia: A Pilot Study,” Australasian Journal on Ageing, April 26.
Puszko, Sharon. 2007. “The Marvelous Benefits of Geriatric Massage,” http://www.thehealthyplanet.com/june07_the.htm.
Rowe M, Alfred D. 1999. “The Effectiveness of Slow-Stroke Massage in Diffusing Agitated Behaviours in Individuals with Alzheimer’s Disease,” Journal of Gerontological Nursing, 25:22–34.
Saczynski, J. S. 2010. “Depressive Symptoms and Risk of Dementia: The Framingham Heart Study,” Neurology, 75:35–41.
Smallwood, J., et al. 2001. “Aromatherapy and Behaviour Disturbances in Dementia: A Randomized Controlled Trial,” International Journal Geriatric Psychiatry, 16:1010–13.
Song, Xiaowei, Arnold Mitnitski, and Kenneth Rockwood. 2011. “Nontraditional Risk Factors Combine to Predict Alzheimer Disease and Dementia,” Neurology, 77:227–34.
Suzuki, Mizue, et al. 2010. “Physical and Psychological Effects of 6-Week Tactile Massage on Elderly Patients with Severe Dementia,” American Journal of Alzheimer’s Disease and Other Dementias, 25:680–86.
Tuesday, June 7, 2011
Turn That Frown Upside Down: In a Massage Face Cradle
Anyone who has ever had a massage can probably attest to how good it makes you feel, both physically and psychically. So the assertion that massage is helpful in combating depression may seem intuitive. But of course, depression is more serious than simply being grumpy or having a bad day: clinical depression, according to the National Institutes of Health’s Medline Plus, “is a mood disorder in which feelings of sadness, loss, anger, or frustration interfere with everyday life for an extended period of time” (emphasis mine). In that light, claims of massage being beneficial in treating depression should not be made lightly.
But it would seem that there is a growing body of research to support this belief. A group of researchers from a university in Taiwan examined seventeen studies on depression and massage and concluded that, while further study is warranted, “massage therapy is significantly associated with alleviated depressive symptoms.” If you’re wondering how massage alleviates these symptoms, it may have to do with, at least in part, the apparent influence of stress.
Research suggests that stressful experiences might deplete such neurotransmitters as dopamine and serotonin. Serotonin modulates mood and emotion, while dopamine plays a role in emotional response and the ability to experience pleasure and pain. Given the types of signals these chemicals transmit across the nervous system, it is easy to see how having less of them might lead to depression. Also, stress increases production of the hormone cortisol, not coincidentally often referred to as the stress hormone. Current research has found that high levels of cortisol are involved in the development of certain depressive disorders, though the mechanism for that development is as yet not understood.
When you get a massage, you can feel the stress melting away. But as you might have gathered by this point, this sensation is not simply psychosomatic. Studies that have analyzed blood and/or urine samples have found that dopamine and serotonin amounts went up and cortisol levels were lower following massage. In addition, massage causes the body to release oxytocin—also known as the “trust hormone”—which would give depression sufferers, among others, an enhanced sense of security.
Studies to date have not researched whether massage would have to be ongoing in order for the benefits to persist. But it’s almost impossible to get too many massages, so it certainly couldn’t hurt to err on the side of caution and get massages as often as time and budgets allow!
Sources
Anisman, Hymie, and Robert M. Zacharko. 1982. “Depression: The Predisposing Influence of Stress.” Behavioral and Brain Sciences 5:89–99.
Field, Tiffany, et al. 2005. “Cortisol Decreases and Serotonin and Dopamine Increase Following Massage Therapy.” International Journal of Neuroscience 115:1397–1413.
———. 2004. “Massage Therapy Effects on Depressed Pregnant Women.” Journal of Psychosomatic Obstetrics and Gynecology 25:115–22.
Hou, Wen-Hsuan, et al. 2010. “Treatment Effects of Massage Therapy in Depressed People: A Meta-Analysis.” Journal of Clinical Psychiatry 71:894–901.
Sher, Leo. 2004. “Daily Hassles, Cortisol, and the Pathogenesis of Depression.” Medical Hypotheses 62:198–202.
Sunday, May 29, 2011
Trademarked Massage
The road to fame and fortune—if that’s what it can be called in this line of work—seems to be to “invent” your own kind of massage. “Invent” in quotation marks because, by and large, new types of massage are actually more like songs using sampling—that is, taking a portion (or a sample) of an already recorded sound or song and using it in the creation of another song. So, for instance, Structural Energetic Therapy (SET) is a combination of deep tissue massage, myofascial release, and kinesiology, developed by massage therapist Don McCann in 1983, while polarity massage therapy, created by Randolph Stone, a doctor of osteopathy, chiropractic, and naturopathic medicine, blends energy-based bodywork, diet, exercises, and self-awareness techniques.
Many of these specialized therapies are referred to by a handy acronym/abbreviation: in addition to SET, there are also, for example, NMT (neuromuscular technique), PUSH (power under soft hands), ART (active release technique), and BART (bonding and relaxing technique). Even therapies that aren’t known by their abbreviation use acronyms to summarize their technique, a practice sometimes inelegantly applied as in SCRIBE, which describes the “six guiding principles” of Comfort Touch (created by Mary Kathleen Rose): Slow, Comforting, Respectful, Into the center, Broad, and Encompassing. I say inelegant in that “into the center,” for example, seems rather contrived, phrased in such a way merely to make the acronym come together. “Inward” might have worked equally well and wouldn’t rely on a preposition to make an intelligible acronym. I have other issues with this summary as well (shouldn’t all massage, for instance, be respectful?), but it’s the infelicity of the prepositional device that strikes the most strident chord with me.
Other therapies avoid the confusion of these helpful, easy to remember abbreviations by their creators’ dispensing with modesty and naming their modalities for themselves: the Arvigo Techniques of Maya Abdominal Massage (for Dr. Rosita Arvigo), Aston-Patterning (for Judith Aston), The Feldenkrais Method (for Dr. Moshé Feldenkrais), The Niel-Asher Technique (for Dr. Simeon Niel-Asher), and Bonnie Prudden Myotherapy (named for—guess who?), among others. Further, many of these are actually trademarked techniques, lest anyone think to borrow wholesale from them and call it their own.
So I’ve been thinking about jumping on the bandwagon and coining my own therapy. The only thing I can’t decide is whether to incorporate my name into the name of the technique: Zipter Catch and Release Technique or just Catch and Release Technique. CRT is nice and simple, but if it has a ring to it, it’s because it’s also the abbreviation for cathode ray tube. ZCRT avoids that but is rather clumsy. CRMT (for Catch and Release Massage Technique)? Maybe I should leave decisions about what to call it, for now, and work, instead, on describing this astonishing new modality.
An acronym summarizing the technique might be a reasonable place to start. And going with the catch-and-release metaphor, I’m thinking FISH might be a nifty mnemonic: Find, Isolate, Squish, Hold. In other words, Find the area of pain, Isolate the knot, Squish the knot, and Hold it until it releases. If that sounds a lot like trigger point therapy, well, in fact, it is. But I mix in a certain je ne sais quoi. It’s the je ne sais quoi part that troubles me, though, in terms of making this a viable technique that can be taught to others. This je ne sais quoi has something to do with intuition, which I’m pretty sure can’t be explicated in a step-by-step way, thereby making it something hard to pass on. Intuition can be developed, I’m convinced, in someone who is open to it and who has a good foundation from which they practice. I’m just not sure how to tell you how to go about acquiring it.
I have therefore reached the unavoidable conclusion that, sadly, my new and would-be patented form of massage is not quite ready for primetime. And to be honest, I just don’t have the chutzpah to claim that what I do is either unique or better than what’s already out there. This isn’t to say that I don’t think I’m a darn good therapist, with special skills and genuine ability. I’m just not ready to proclaim myself a new massage messiah.
Plus, there are already a lot of good modalities out there, with each having their appeal and benefit for different people for different situations in their lives. For instance, though I’ve made light of Comfort Touch’s SCRIBE mnemonic, that type of massage is actually quite beneficial for those who are frail and/or ill. And its creator has generously answered many of my questions, without knowing me from Adam. I think my point here is—and, to quote Ellen DeGeneres, I do have one—that it’s important to shop around not only for a massage therapist but also for modalities so you can find the one that’s right for you right now.
But with something like 160 modalities currently in use and with an estimated 278,000 massage therapists in the United States as of January 2008, the task of finding that right therapist seems daunting to say the least. That’s a stress producer right there! But for help finding a massage therapist, while nothing beats a recommendation from a trusted friend, a good place to start searching for someone that specializes in a particular modality are the registries of the two professional massage associations and the national certification board.
As for me, fame and fortune may not be in the cards but—and I apologize for sounding like a sap—the thought that I will have an opportunity to help make people feel better, every day, for years to come, is a reward in itself. And I’m sure that’s how the bank that holds my mortgage feels as well.
Sources:
On the number of modalities, see http://www.massage-therapy-benefits.net/types-of-massage-therapy.html.
For numbers of massage therapists: http://www.massagetherapy.com/media/metricsgrowth.php.
The registries for the professional associations and certification board can be found at http://www.amtamassage.org/findamassage/index.html, http://www.massagetherapy.com/find/., and http://www.ncbtmb.org/consumers_find_practitioner.php.
Thursday, May 12, 2011
Contents under Pressure: Massage for Hypertension?
All manner of assertions are made about the benefits of massage. But are they all true? And how do we know?
It used to be that everything we knew about massage was based on anecdotal evidence and observation. As scientists have learned more about the how the human body functions, however, and as interest has grown in complementary and alternative therapies, researchers have started to examine some of the claims made for massage. It is frequently alleged, for instance, that massage can reduce blood pressure.
This claim is, of course, relatively easy to test. Blood pressure can be checked, using a blood pressure cuff, before a massage and then again afterward. If someone’s blood pressure is lower for the after measure and there were no other variables, it seems pretty clear that massage was responsible for the change—especially when these results are replicated numerous times with numerous subjects.
And, in fact, a variety of studies have shown that massage lowers both diastolic and systolic blood pressure. (Diastolic, as you may recall, refers to the pressure between beats, or when your heart is at rest, whereas systolic is the pressure during a heartbeat and is higher than the diastolic pressure.) A study that looked at the effects of a relaxing back massage on hospice patients found not only that blood pressure was lower following the massage but that it actually continued to decrease when they measured again, several minutes later. Even a five-minute hand massage has been shown to lower blood pressure significantly.
It appears, however, that not every kind of massage has this effect on blood pressure. For instance, researchers at the National University of Health Sciences in Lombard, IL, examined the effect of different types of massages on blood pressure and found that recipients of trigger point therapy (in which sustained pressure is applied to a knot to help it release) and sports massage (a vigorous massage using a variety of techniques) had, in fact, higher blood pressure just following treatment. This is not surprising when you consider that intensive therapies such as these can sometimes create temporary discomfort and, further, when you consider that acute pain has been shown to lead to a surge of adrenalin, which in turn increases heart rate and blood pressure. But as soon as adrenalin levels fall back to normal, so do heart rate and blood pressure. Assuredly, though, neither of these types of massage would be good choices if your goal was to lower blood pressure. Then again, relaxation and stress relief are not the intent of such massages.
For something like Swedish massage, though, which does lower blood pressure, how does it do so? Massage, as it turns out, causes a decrease of the hormone arginine vasopressin (AVP)—which constricts blood vessels and raises blood pressure. The test subjects for the research demonstrating this submitted to having blood drawn numerous times before and after the massage via catheters inserted into the arm for the duration. This fact makes the results even more impressive, given that getting a forty-five-minute massage with a needle poking into your arm is not an entirely stress-free circumstance.
While lowering blood pressure is, in and of itself, a good thing, when you take into consideration that high blood pressure is linked to elevated measures of stress, anxiety, the “flight-or-fight” hormones known collectively as catecholamines, depression, and hostility, reducing blood pressure levels takes on even greater importance. Massage may not be “just what the doctor ordered (yet)—but it should be! Massage: it does a body good!
Sources
Aourell, Moa, et al. 2005. “Effects of Swedish Massage on Blood Pressure.” Complementary Therapies in Clinical Practice 11:242–46.
Cambron, Jerrilyn A. 2006. “Changes in Blood Pressure after Various Forms of Therapeutic Massage: A Preliminary Study.” Journal of Alternative and Complementary Medicine 12:65–70.
Cloud, John. 2011. “The Lab Rat Gets Petted: How Massage Works.” Time.com, January 19.
Fraser, Joy, and Janet Ross Kerr. 1993. “Psychological Effects of Back Massage on Elderly Institutionalized Patients.” Journal of Advanced Nursing 18:238–45.
Hernandez-Reif, Maria, et al. 2000. “High Blood Pressure and Associated Symptoms Reduced by Massage Therapy.” Journal of Bodywork and Movement Therapies 4:31–38.
Kaye, David Alan, et al. 2008. “The Effect of Deep-Tissue Massage Therapy on Blood Pressure and Heart Rate.” Journal of Alternative and Complementary Medicine 14:125–28.
Kim, Man Soo, et al. 2001. “Effects of Hand Massage on Anxiety in Cataract Surgery Using Local Anesthesia.” Journal of Cataract and Refractive Surgery 27:884–90.
Meek, Sandra S. 2003. “Effects of Slow Stroke Back Massage on Relaxation in Hospice Clients.” IMAGE: Journal of Nursing Scholarship 25:17–21.
Monday, April 11, 2011
Taking a Tiny Tumble
Late evening massage gigs when traveling by cargo bike—a bakfiets, in my case—is not without its hazards.
I recently was hired to do chair massage at a cocktail party fundraiser for a local parochial school. The guests would be moms whose kids attended the school, and I, along with one of my massage therapist friends, would be providing short massages for the guests in between their eating, drinking, and socializing. The massage portion of the party was going to be offered from 7 pm until 10 pm, and though I was a little leery of traveling five miles on a bike with my massage chair in tow after 10 at night, not only were the brakes on my car beginning to fail but, also, one of the guests at the party was the host of the show 190 North, where I’d been featured as a massage therapist who delivered massage “on two wheels.” It therefore seemed wrong, somehow, to arrive on four wheels.
Getting there was no problem, since at this time of year there is plenty of daylight at 6 or 7 at night. My biggest problem was trying to ride slowly enough that I didn’t arrive sweaty. I am not the type of cyclist to just tool along, even when I’m not in a hurry. Actually, I’m not the type of walker, swimmer, etc. to go slowly. Sometimes I think doing massage—which generally requires a measured pace—is therapy for me. But I somehow managed to arrive not requiring a shower and change of clothing.
More challenging was the getting home. To begin with, I am usually in bed by 10. But here I was, at 10, not only upright but actually packing up my massage chair and readying myself to ride home. I was so tired by then—having earlier in the day gone for a short run with the dog and attended my two-year-old niece’s birthday party—that I could barely form coherent sentences. But after a tiny lemon tart for the road from one of the hosts, I trundled my massage chair to the end of the block where I’d locked up the bakfiets, loaded the chair into the box of the bike, zipped up my jacket, put on my helmet, and headed down the street toward home, sweet home.
I had gone hardly more than a block or two, though, when I realized that while it wasn’t really cold out, there was enough wind that, without the little hat I’d brought along, my ears were going to be unhappy with me. So I found a safe spot to stop on a side street, put down the kickstand, and rummaged through my bag for my hat. After I’d put on the hat and rebuckled my helmet, I climbed on the bike, ready to set off again, only then realizing that I’d forgotten to put up the kickstand.
Now the kickstand on the bakfiets is not some slender metal wand beside the pedal to which you can apply a simple kick backward with the heel to make disappear. In order to hold a hundred pounds of bike up in a steady fashion requires something more substantial, and the kickstand for the bakfiets has two rubber-tipped feet on either end of rod that runs beneath the box. Putting the kickstand up requires giving the bike a good push forward to take its weight off the stand and then looping your toes behind one side of the stand to slam the feet up into a locked position.
I blame it on the fact that I was tired, for I don’t know what else could have possessed me to think I could do all of that while straddling the bike frame. Pushing the bike forward went fine, but when I went to flip the kickstand up into the locked position, my pants leg got caught on one of the feet—just as the kickstand locked into place, of course. The only way to let the kickstand down again is to tap the coin-sized lever just to the right of where my leg was now fairly firmly trapped. And before it even happened, I knew the only way out was down. And that’s where I went: me, the massage chair, and my bag, all dumped on the ground as the bakfiets tumbled over.
Other than a slight scrape on the left palm and a rather savage nudge in the butt from my bike seat, I was unhurt. But wouldn’t you know it: just as I and my things spilled out into the road, a car came along. Off to the side, as I was, I was in no danger of being run over—just of being really embarrassed. I swiftly righted the bike, put the kickstand in place (which had come down in the fall), reloaded, and got back on. The car sped off without so much as an “are you ok?” Which was fine with me. I wasn’t keen on acknowledging my klutziness, thereby more firmly entrenching the embarrassment.
The rest of the ride was less eventful, but suffice it to say, there is a different feel to riding your bike down the street at 10:30 on a Saturday night than there is during the daylight. First there were the Saturday date-night folks, going to or from trendy bars and restaurants in the Lincoln Square area. Then, on Lawrence Ave., I saw a man standing on the sidewalk wrapping himself in a long white cloth, perhaps a dhoti. I’d never seen anyone in the process of doing that, much less on the sidewalk, so that was interesting. But the crowd in front of the Admiral Theater with its euphemistically named adult entertainment just made me sad, seeming to be, as the song says, “looking for love in all the wrong places.”
But then who knows: they might have thought I was the one to be pitied, a poor woman alone on a Saturday night on her weird bicycle! Little did they know that the next day I’d be out with my best gal at the garden center, buying some window-box plants and a bale of straw for the garden. Oh yeah, I’m a happenin’ gal. Don’t cry for me, Admiral Theater.
Saturday, March 26, 2011
How'd I Get That Pain? Part 3, Limbs
As noted in part 1 of this article, there are times when there is little doubt about why you have a particular pain. But if you have a muscle pain that seems to come from nowhere, factors such as those listed in the article linked to below might be responsible—factors that could be avoided in the future. Of course, when you can’t dodge an ache, it’s time to see your massage therapist! Calf pain? An ache in your forearm? Hamstrings killing you? You might have gotten that soreness this way:
| Muscle | Location | Stressors of That Muscle |
| Extensors | Top (or hairy side) of the forearm, from the outer edge of the elbow to the base of each finger | Repetitive forceful hand gripping and repetitive extension; weeding with a trowel, extensive handshaking, or Frisbee throwing; faulty mechanics (e.g., typing playing musical instruments) |
| Flexors | Inside (or nonhairy side) of the forearm, from the inner edge of the elbow to the base of each finger or the base of the palm | Prolonged gripping or grasping (e.g., working with hand tools, racquet sports); being in professions such as massage therapy, carpentry, weight lifting, waiting tables, chefs |
| Pronator teres | Around the inner side of the elbow | Gripping ski poles for long periods of time; holding small hand tools lightly |
| Supinator | Above and around the outer part of the elbow to the nearest third of the radius from there | Repetitive or sustained supination (rotation in which palm faces upward) of hand, especially with elbow straight as in “flipping” a briefcase onto a table, wrestling with a stiff doorknob, mis-hitting a ball off-center, twisting a racquet with elbow completely extended, wringing clothes; opening jars, working with a screwdriver |
| Triceps brachii | From the top, back of the shoulder joint to the back of the elbow | Strain from sports (e.g., “mis-hit” tennis ball or improper golf swing); overuse of forearm crutches or a cane that’s too long; prolonged extension lacking elbow support (e.g., holding down a sheet of paper while writing or doing needlepoint work); push-ups or overhead and bench presses |
| Brachioradialis | Top of the outer edge of the upper arm to the far outer edge of the radius | Combining gripping and twisting motions as in sports (tennis and other racquet sports) |
| Brachialis | From about midway down the inside of the upper arm to the front side of the top of the ulna | Heavy overload from lifting (e.g., holding a power tool or meticulous ironing) |
| Biceps brachii | From the inner side of the scapula to the inside of the elbow | Unaccustomed vigorous repeated supination (e.g., using a screwdriver); lifting heavy objects with the hand supinated; sustained elbow flexion (e.g., playing a violin or guitar, using electric hedge clippers) |
| Peroneals | Upper outer edge of the fibula to behind the outer edge of the ankle | A fall with twisting and turning inward of the ankle; weakness from prolonged underuse (e.g., being in a cast or mostly sitting day and night); lower leg length inequality; poor arches; pronated feet |
| Flexor digitorum longus and flexor hallucis longus | Down the back surface of the tibia to the sole of the foot and the base of the big toe, respectively | Hyperpronation or an unstable foot; a badly worn shoe (esp. with runners) that creates an unstable gait; an inflexible shoe sole that prevents normal extension of the foot and toe joints during walking or running; walking and running on sand, especially barefoot |
| Tibialis posterior | Underneath the soleus and gastrocnemius muscles | Running on uneven surfaces or being new to running; excessive pronation; footwear that is badly worn or encourages turning the foot outward or rocking |
| Extensor digitorum longus and extensor hallucis longus | Along the shin bone to the start of the toe bones on the top of the foot | Steep accelerator pedal in a car; sitting for long periods with the feet back under a chair; nervous twitching of the foot |
| Tibialis anterior | From the top of the outer edge of the tibia to the top of the foot | Catching the toe on an obstruction; overuse, such as during running (leading to shin splints) |
| Popliteus | From the outer surface of the lower end of the femur to the top of the back of the tibia | Excessive pronation; playing soccer or football, running, twists or slides, especially when running or skiing downhill; tearing of the posterior cruciate ligament |
| Soleus | Long flat muscle under gastrocnemius | Wearing high heels, slipping or losing balance; sitting in a chair that is too high; too tight and/or high stocking or elastic-band socks that may limit blood supply; ice skating, roller blading, or skiing without good ankle support; lower leg length inequalities |
| Gastrocnemius | From the inner and outer surfaces of the bottom of the femur to the back of the heel | Physical overload and/or bad positioning of the foot (e.g., climbing steep slopes, riding a bicycle with the seat too low, wearing a cast on the leg); wearing high heels, prolonged driving in a car, certain sleep positions |
| Pectineus | From the base of the pubic bone to the top of the inner side of the femur | Lower limb length inequality; horseback riding, gymnastics, soccer (running and kicking at the same time); sitting cross-legged; sitting with the hips in a jackknifed position |
| Adductor brevis and longus | From the lower edge of the pubic bone to the upper inside edge of the femur | Strenuous horseback riding, in-line skating, cross-country skiing; sitting in a fixed position with hips acutely flexed and on thigh or leg crossed over the other knee |
| Adductor magnus | The large triangular muscle that starts at the lower inside edge of the pubis and attaches the base of the butt and the inside of the femur | Sitting in chairs for long periods; chronic hamstring strain and fascial distortion; pelvic misalignment; lower leg length inequality |
| Sartorius | From the front of the outer edge of the hipbone to the upper inside part of the tibia | Prolonged sitting in a cross-legged “tailor’s” position; excessive pronation of the foot |
| Gracilis | From the lower part of the pubis to the inner side of the knee | Slipping and resisting spreading legs while trying to recover balance; overenthusiastic exercising; structural knee dysfunction; postural imbalance |
| Vastus muscles | From the top of the inner and outer edges of the femur to just below the knee cap | Pronated arch; structural misalignment in the pelvis; imbalance between vastus lateralis and vastus medialis |
| Rectus femoris | Top of the front of the thigh to top of the knee cap | Jumping, running downhill, skiing, weight lifting, deep knee bends; lordosis (when the spine curves outward at its base; a swaybacked posture) |
Thursday, March 10, 2011
My Bread and Barter
Bartering—the exchange of goods or services between two parties for mutual advantage—predates the use of currency and has probably been around since the dawn of humankind. It has even been argued that if symbiotic relationships are construed as a form of bartering, plants and animals engage in bartering as well.
According to “The History of Money,” a PBS online article from NOVA (www.pbs.org/wgbh/nova/moolah/history.html), “Cattle, which include anything from cows, to sheep, to camels are the first and oldest form of money”—though it’s hard to imagine the kind of purse you’d need to carry a cow or how you’d get change for a camel! But even when metal coins first appeared in China around 1000 bc and then elsewhere, such as Greece, Turkey (then known as Lydia), and Persia, around 500 bc, not everyone had access to coinage, and bartering continued to be a common way for people to get things they needed in exchange for things they had. We should all be glad, in any case, that tax misdeeds are punished, today, only with fines or jail time—unlike the Danes that lived in Ireland around ad 800–900 who, if they failed to pay the Danish poll tax, had their noses slit—hence the phrase “paying through the nose”!
The overlap of bartering and currency-based economies has never ceased entirely. However, despite former Nevada state GOP chair Sue Lowden’s recent suggestion that health care costs be lowered by having people barter with their doctors (which I’m sure would be ever-so-appealing to your HMO or PPO!), bartering has decidedly not been a primary means of obtaining goods and services for people in this country for quite some time. Our current economy, though, in which money can be as hard to come by as a pocketful of sheep, has caused a resurgence of bartering.
And given this climate, I have to say that having something like massage to trade has come in very handy. I am, I think I can safely say, the envy of all my friends in fields like academia, social work, and data processing. For the most part, I’ve traded massage for personal training sessions, but I have also traded for construction work on my home, design work for my business, and getting a handmade belt made for my kickass Monster Half-Marathon finisher’s belt buckle. Theoretically, I have editing and writing services to barter as well, but frankly, not only do people have much less need for those (or think they do!), but having your punctuation checked is far less alluring to most folks than getting your stress relieved.
There are limits, of course—it’s not like I can offer a massage to someone at AT&T in exchange for some phone service or at Jewel Foods for bread and milk. But small businesses of all manner, as well as individuals, seem open to the idea of doing trades. And for me it’s been a huge help with getting some of the things I need or want that I wouldn’t have been able otherwise to afford right now.
Making sure the trades are fair to both parties is potentially tricky, but so far, using my hourly massage rate as a gauge has made it relatively easy to ensure equity. It also bears considering whether something like massage can ethically be traded for certain kinds of services, especially when there is an ongoing relationship with those you hope to trade with. For instance, I think you’d have to question the professionalism of any psychotherapist who was willing to trade counseling for massage—boundary issues spring to mind. . . .
But in the main, having a spare massage in my wallet to use for “buying” certain goods and services has been great. It really is win-win. And right now I’ve got my eye on a birch sapling over at the local garden center. Not sure how many massages it would cost (or even if they’d be willing), but whatever the price, it would be worth it just to drive the sapling home in the box of my cargo bike!